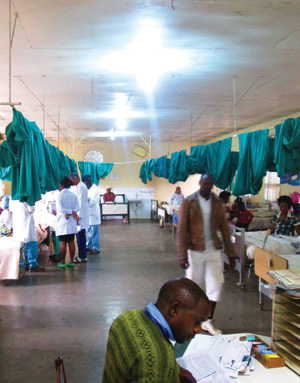
Capstone projects open doors to helping the medically underserved
Jeremy Powers, M’14, was driven by one thing and one thing only when he entered medical school in 2010. Like many of his classmates, his main mission in life was, and continues to be, helping people.
Especially the underserved.
“I feel drawn to helping those people from an underserved area,” he said.
So when he began considering his options for medical school, he immediately was drawn to the MCV Campus, in large part because of the school’s International/Inner City/Rural Preceptorship (I2CRP) Program.
All medical students can apply to the four-year program. It fosters the knowledge, skills and values needed by doctors to provide quality and compassionate care to the less fortunate.
A major focus of the program comes during the final year, when students complete a community-based capstone project. Each project has the potential to help communities – local, elsewhere in the U.S. or overseas – by addressing critical medical needs. It gives students the opportunity to serve patients before they even graduate from medical school.
“I feel very proud to have been part of this,” said Powers, who traveled to Cameroon to complete his capstone project. “It provided me with a way to focus on the things that drew me to medicine in the first place.”
Other schools across the country have programs similar to I2CRP, but VCU’s offering is unique in that it runs for four years, allowing classmates to remain together as they share life-changing experiences.
“The nature of the training is invaluable,” said Mark Ryan, M’00, H’03, medical director of I2CRP.
Ryan was one of just two students to be part of I2CRP’s first graduating class in 2000. At that time, the program focused on inner-city and rural communities. The international element was added in 2007.
“It started small as a test program,” said Ryan, assistant professor for the Department of Family Medicine and Population Health. “Now, it is getting increasingly competitive. The quality of students who are not accepted is remarkable. It’s really hard to make that final cut.”
This year, 69 students applied for 24 spots.
“There is more and more interest each year,” said Ryan, who leads the program alongside assistant professor Mary Lee Magee, M.S., who serves as I2CRP’s educational director. “My sense is there is a generational component to it,” Ryan said. “There is a generational movement to serving others.”
I2CRP students participate in community volunteer activities, monthly journal club meetings and annual elective courses designed to foster a deeper understanding of underserved populations. Students also complete semester-long rotations in underserved settings during their first- and second-years.
By their third year, students spend a total of 10 weeks in underserved communities during rotations in family medicine, general internal medicine, pediatrics and general surgery.
“These students are not just in the program because they have great credentials,” Ryan said. “They are here because they have heart.”
Ryan himself was attracted to the idea of helping the underserved after spending a weekend on the Eastern Shore during his undergraduate studies at William & Mary.
“Driving around rural Virginia, I began recognizing the barriers people there had to accessing health care,” he said. “There was a level of need that was compelling to me.”
Most I2CRP students come into the program with a long list of volunteer hours already logged. Many have completed mission trips overseas, spent weekends in this country at rural clinics or traveled with church members during summer vacation to provide health care to the poor and homeless.
“There’s a different level of visibility today on the part of students in terms of the roles they can play,” Ryan said. “There is so much more awareness. They know they can do meaningful things. They want to step in and do their part.”
Take a look at four recent capstone projects that are bringing change to underserved communities locally and around the world.
Capstone project shapes life’s direction – Jeremy Powers, M’14
Interpreting what’s best for patients – Scott Toney, M’15
Alerting Latinos and other minorities to skin cancer risk – Ashley McWilliams, M’15
Capstone project shapes life’s direction
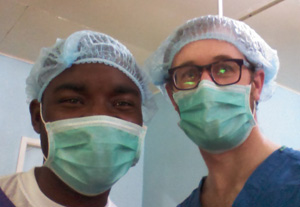
Jeremy Powers, M’14, traveled to Cameroon last year to find out if general surgery residents there could provide better care to patients if they had training in plastic surgery. The answer? A resounding yes.
“What walks through the door there is what they have to deal with, whether they have the training or not,” Powers said. “They see a lot, and a lot goes untreated because the expertise is not there.”
Patients may present with burns, soft tissue cancer, facial deformities, open wounds or other injuries that could benefit from plastic surgery but don’t, because the few surgeons who do practice in Cameroon don’t have the needed training.
“There are huge social and self-esteem issues associated with these types of cases,” Powers said. “Plastic surgery can often restore form and function, providing patients with a better quality of life.”
Medical care is hard to come by in Cameroon, where the doctor-to-patient ratio is about 1 to 15,000. Plastic surgeons are even more scarce.
That’s why Powers developed a survey and met with eight general surgery residents as part of his project. Because of the types of injuries these surgeons see and because specialists in plastic surgery are rarely available, all agreed more training would benefit patients.
“They want as much training as they can get, not just in plastic surgery, but in other areas as well, from experts in the field,” Powers said. “Medical aid is no longer simply about providing services to the underserved. In fact, if we just did that we may be doing a disservice to these communities, perpetuating a sense of dependency. We now have the opportunity to equip and train the brilliant and talented people who are already there with a heart to serve their own people.”
Powers graduated from William & Mary in 2009 and taught high school calculus, European history, physics and trigonometry before entering medical school to “make a positive difference in the world.” He remains at VCU as a resident in plastic and reconstructive surgery, and plans to one day practice and teach in underserved communities.
“My motivation comes from my faith, as Jesus teaches us to serve the poor,” Powers said. “I2CRP has taught me so much. I know that what I’ve learned will continue to serve my patients throughout my entire career.”
Interpreting what’s best for patients
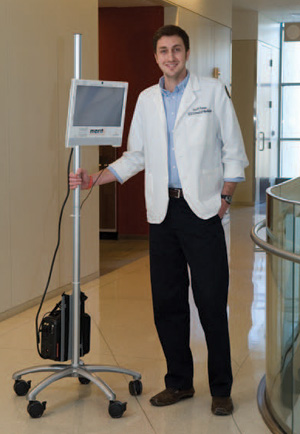
Scott Toney, M’15, will never forget the frightened teenager who had been rushed into the emergency room. Doctors tried to explain the injuries he had suffered when he fell off the roof, but they weren’t sure he understood the fact that surgery would be necessary to stop the internal bleeding.
“He did not speak English,” said Toney, who was on surgical rotation that day during his third year of medical school. “It became apparent that he did not fully understand the gravity of his injuries.”
With the memory of that experience still vividly in place, Toney examined interpretation services in the inpatient setting as part of his capstone project. He wanted to know if the type of interpretation method affects patient and provider satisfaction and if certain interpretation methods are more appropriate in certain clinical scenarios.
“I want the patients at VCU who are not English speaking to receive the best possible care,” he said. “We have interpretation services available, and by law we must provide them. But which method is best?”
The VCU Medical Center averages five to 20 Spanish-speaking patients on any given day. Health care providers can call on live interpreters to visit patients and translate for them or use technology assisted interpretation that are phone or web based.
“With the live interpreters, patients build a trust,” said Toney, who is headed to the Naval hospital in San Diego to begin his residency in pediatrics. “But as society becomes more tech savvy, patients are growing more comfortable with that as well.”
Toney, who grew up in Atlanta, has an undergraduate degree in health science from James Madison University. He is no stranger to visiting the underserved, having taken 10 mission trips to such places as Mexico, Peru, Ecuador, El Salvador and the Dominican Republic.
“To see other places in the world that don’t have the freedoms and the resources we have here is incredibly humbling,” he said. “It has motivated me to treat everyone with the utmost respect. I’ve come to realize that everyone has the same wants and desires. Everyone wants to be healthy.”
Alerting Latinos and other minorities to skin cancer risk

“There are misconceptions out there that people with darker skin won’t get skin cancer,” said Ashley McWilliams, M’15. “That simply is not true.”
As part of her capstone project, McWilliams made it her mission to raise awareness.
“As the population of Latinos continues to increase, we need to target that population or there will be an increase in skin cancer cases,” she said. “We must get in front of the problem.”
According to the Skin Cancer Foundation, skin cancer rates among Hispanics rose by almost 20 percent in the United States in the last two decades. And since Hispanics are the fastest-growing population in the U.S., McWilliams cautions, the number diagnosed will only continue to rise.
To increase awareness, McWilliams surveyed minority patients at a local clinic to assess their knowledge and perceptions of melanoma, including risk factors associated with this form of cancer, their ability to recognize the early stages of melanoma and their willingness to have a suspicious spot examined by a physician.
“When melanoma presents in minorities, it presents differently,” McWilliams said. “For Caucasians, it presents on the face, neck and chest. For persons of color, it usually presents on the palms and soles of the feet as well as underneath fingernails or toenails. And the outcome is not as good in these groups compared to Caucasians.”
Her project not only helped educate minorities about skin cancer, but it also gave physicians a better understanding of their patients’ points of view. Because some patients feel they are not at risk, for example, they don’t think it is necessary to talk with doctors about a change in their skin’s appearance, chalking it up instead to aging or some other factor. Physicians, therefore, should discuss the risks and the warning signs.
“It was really a quality improvement study,” said McWilliams, who is headed into her surgery intern year at the VCU Medical Center. “The more knowledge patients and providers have, the better our quality of care.”
McWilliams, who grew up in Pensacola, Fla., received her undergraduate degree in biology from Howard University in 2008. She worked in research and health policy for a few years before entering medical school.
“I wanted to interact more with patients and help educate them in the healthiest ways to live their lives,” she said.
Her interest in dermatology dates to her middle school days.
“My science fair project examined which brand of sunscreen or tanning oil provided the best protection from the sun,” she said. “Of course we all know now that tanning oil doesn’t provide any protection at all, but the project demonstrated to me how the lack of proper protection from UV rays can cause lots of damage to your skin and over time can increase your chances of developing skin cancer.”
It also opened her eyes to the importance of skin cancer prevention. “The odds might not be as high that a person of color will get skin cancer,” she said. “But if we can educate and in the process save one life, that’s the most important thing.”
Breaking down the barriers to good health

The challenges of caring for the underserved are many. Communication. Transportation. Trust. Physicians can’t always get a clear picture of what’s going on in the lives of their patients.
To help sharpen the view in one underserved area, the Class of 2015’s Heather Root, Lauren Clifford and Gordon Pace traveled to Lima, Peru for 10 days to uncover the roadblocks many face to achieving good health.
“When physicians get to know the whole patient, they can provide a higher quality of care,” said Root, who’ll begin her internal medicine residency at Emory this summer. “I welcome that challenge.”
The group teamed with the family medicine residents on site to survey local neighborhoods. They went door to door, asking family members about their backgrounds, daily diets, lifestyles, family medical histories, neighborhood crime and more.
“What was nice was how closely we got to work with the medical residents,” Pace said. “They welcomed us right in.”
The group visited more than 100 homes during their stay. They plan to analyze the information they gathered to see if correlations can be made between a person’s home life and their health care.
“We’ll look at those who have been vaccinated, for example, and those who haven’t and cross-reference that with those who have insurance and those who don’t,” Clifford said.
They will share their findings with the medical staff they worked with. They hope this study will be the first of many.
“What excites me is the idea of a cross-cultural partnership,” Pace said. “This was such an exceptional experience, I would love to see it continue.”
Traveling out of the country is nothing new for Pace, Clifford and Root. All three had experience working in Central America as part of the I2CRP and HOMBRE (Honduras Outreach Medical Brigada Relief Effort) programs. They also have done mission work on their own.
“While volunteering in rural clinics, I’ve seen the sickest of the sick and the poorest of the poor,” said Clifford, who has an undergraduate degree in art history from William & Mary. “I’m always shocked by how the people most in need are the ones who aren’t getting it. That has spurred me to do what I can to serve.”
Clifford, who is set to begin her pediatrics residency at the Medical University of South Carolina, is following in her father’s footsteps by becoming a doctor. She counts her experience with the I2CRP program as one of the most important of her life.
“I feel like this is something every single physician should be exposed to,” she said. “It has been a true privilege.”
Pace, who earned his undergraduate degree in history from Mississippi State University in 2003, took a few years off after school to volunteer in Belfast, Northern Ireland, where he worked with inner city youth. He also spent time in Arizona working with immigrants. He is headed to Yale New Haven Hospital for a residency in internal medicine.
“It’s interesting to go to different metropolitan areas around the world and compare nutrition and other cultural elements,” he said. “When we were in Peru, one minute we were surveying the poorest residents, and then within walking distance we saw upscale homes.”
No matter the location, people want the same thing – good health.
“The challenge is giving them a clear path to achieving it,” said Root, who has a math degree from Emory University. “When we understand the whole patient and the challenges they face at home, good health care can become more attainable.”
Her trip to Peru reaffirmed that belief.
“Some people may shy away from helping the underserved,” she said. “It can sometimes be complex and frustrating. But I believe that it doesn’t get any better than giving help to those who need it most.”
By Janet Showalter